Did this "Stanford Study" prove that face masks don't slow the spread of COVID-19 and harm the health of mask-wearers? No, that's not true: Stanford University disavows the article, which is not a report on new research and is full of the kind of spelling and grammar errors not found in journals by and for science professionals. It is, as its title says, a hypothesis and not a scientist's report on new data. There is no evidence the claims, written by an exercise physiologist, were reviewed by virologists, pulmonologists or other relevant experts in COVID-19 public health measures. The journal that published it self-identifies as a journal of speculations and radical ideas, not a documenter of new knowledge. The article recycles false claims about mask-wearing, including widely debunked claims of reduced oxygen intake and increased bacterial exposure.
The claims were made in an article (archived here) published by "Medical Hypotheses" January 21, 2021, under the title "Facemasks in the COVID-19 era: A health hypothesis". It opened:
Many countries across the globe utilized medical and non-medical facemasks as non-pharmaceutical intervention
for reducing the transmission and infectivity of coronavirus disease-2019 (COVID-19). Although, scientific evidence supporting facemasks' efficacy is lacking, adverse physiological, psychological and health effects are established. Is has been hypothesized that facemasks have compromised safety and efficacy profile and should be
avoided from use.
This is what the article looked like at the time of writing:
(Source: Medical Hypotheses screenshot taken Tue Apr 20 22:12:24 UTC 2021)
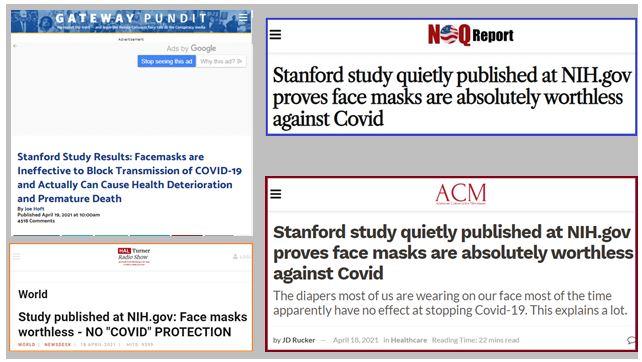
This is how the Medical Hypotheses article was being cited by anti-mask websites at the time this fact check was written, incorrectly crediting Stanford for the study and falsely listing the National Institutes of Health (NIH) as publisher of the hypothesis article:
(Source: Lead Stories montage created from screenshots taken Tue Apr 20, 2021)
The NIH provides PubMed Central (PMC), which is a free full-text archive of biomedical and life sciences journal literature. But the NIH clearly states "PMC is not a publisher and does not publish journal articles itself." Users of PubMed know the website's disclaimer: "The presence of an article in PMC does not reflect an endorsement of, or concurrence with, the contents of the article..."
In an April 20, 2021, email to Lead Stories, Stanford University Medical School senior director of external communications Julie Greicius said Stanford has asked for corrections to those headlines:
A study on the efficacy of face masks against COVID-19 published in the November 2020 issue of the journal Medical Hypotheses is not a "Stanford study." The author's affiliation is inaccurately attributed to Stanford, and we have requested a correction. Stanford University has never employed Baruch Vainshelboim. Several years ago (2015), he was a visiting scholar at Stanford for a year, on matters unrelated to this paper.
Medical Hypotheses is not a research journal
When it announced the new editor in chief of Medical Hypotheses, the journal's owner, Elsevier, said it has a unique purpose, aiming to "... give open-minded consideration to novel, radical new ideas and speculations in medicine which would probably be rejected by most conventional journals."
Merriam-Webster.com defines a hypothesis as an assumption or concession made for the sake of argument, while in science, the word is generally used to describe a prediction that can be tested through experimentation.
Unlike most scientific journal articles, which are carefully edited by professionals, this one is riddled with grammatical, spelling and typographic errors
For example, in the Abstract, a summary that is the most-read part of any journal article, there are punctuation mistakes, spelling errors, misused words, plural nouns in place of singular and the kind of clumsy phrases a scholar's editors would never tolerate in credible journals of science. What follows are screengrabs with unprofessional writing highlighted in yellow.
(Source: Medical Hypotheses screenshot taken Tue Apr 20 at 18:34:57 UTC 2021)
(Source: Medical Hypotheses screenshot taken Tue Apr 20 at 19:00:02 UTC 2021)
In the article's Conclusion section, the other heavily-read part of any article in a science journal, the editors and author repeat errors from the abstract, including "... health organizations should utilize prosper and scientific evidence-based approach with respect to wearing facemasks ..." which should be "proper" and "approaches."
The article repeats false claims that mask-wearing is ineffective and causes hypercapnia and other health problems
The article claims:
facemasks restrict breathing, causing hypoxemia and hypercapnia and increase the risk for respiratory complications, self-contamination and exacerbation of existing chronic conditions
As HealthFeedback.org pointed out in a 2020 fact check by Lead Stories, medical professionals wear masks for much of the day with none of the reduced oxygen intake the article warns of:
While it is true that hypercapnia can be life-threatening, the claim that it can be caused by wearing face masks, either surgical masks or respirators, is unsupported and runs contrary to existing evidence. The masks act as a barrier to keep out aerosols, but the materials used are still porous enough to allow gas molecules like carbon dioxide and oxygen to pass through, which are many times smaller than viruses. The size of a carbon dioxide molecule is estimated at about 230 picometers. In contrast, SARS-CoV-2, the causative agent for COVID-19, is about 60 to 140 nanometers[1], which is at least 10,000 times larger.
The hypothesis article goes on to list the ill-effects of masking up to slow the spread of COVID-19:
Wearing facemasks has been demonstrated to have substantial adverse physiological and psychological effects. These include hypoxia, hypercapnia, shortness of breath, increased acidity and toxicity, activation of fear and stress response, rise in stress hormones, immunosuppression, fatigue, headaches, decline in cognitive performance, predisposition for viral and infectious illnesses, chronic stress, anxiety and depression. Long-term consequences of wearing facemask can cause health deterioration, developing and progression of chronic diseases and premature death.
The Centers for Disease Control and Prevention, which leads public health efforts in the U.S., provides multiple studies and expert reports on the benefits of mask-wearing which refute the hypothesis article's claims that mask-wearers are facing health issues worse than the COVID-19 masks are intended to block.
As of the date this was written, Lead Stories had debunked multiple false claims about unhealthy bacterial buildup in masks, interviewing medical experts and consulting peer-reviewed academic journals for 10 separate fact-checks. The consensus view of trained experts is that mask wearing slows the spread of COVID-19 and, while inconvenient, does little harm to the wearer, especially compared to the health effects of COVID-19 infection.