CORRECTION -- STORY UPDATED: check for updates below.
(Editor's Note: This story has taken off the label "Fact Check" because there continues to be disagreement in the medical, scientific and political fields about the safety and wisdom of lifting lockdowns and restrictions.)
Would allowing everyone, except the most vulnerable, to go on with their lives and forget about the lockdown put an end to the COVID-19 outbreak? No, that's not a safe assumption: The notion of "herd immunity," the idea that letting large numbers of people contract the virus so as to develop immunity and stop the spread, has been shot down by experts who warn of the dangers in this case.
The claim that society has gone about this all wrong and is instead prolonging the problem with the stay-at-home orders, lockdowns and other measures came out of a narrow selection of quotes taken out of a long interview with Knut Wittkowski, an epidemiologist formerly with the Department of Biostatistics, Epidemiology, and Research Design at The Rockefeller University in New York City.
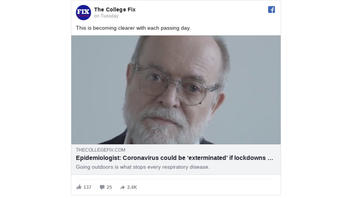
The interview with Wittkowski -- who put out this study -- fueled articles, including one shared by The College Fix in this Facebook post (archived here) published on April 7, 2020. The text above the post read:
This is becoming clearer with each passing day.
And this is what the post looked like on Facebook at the time of writing:
The interview, titled "Perspectives on the Pandemic II: A Conversation with Dr. Knut Wittkowski," inspired write-ups that include one by The College Fix, which describes itself on its Facebook page as "the nation's best source for daily conservative & libertarian campus news."
Attempts to "flatten the curve" will serve to extend the problem, Wittkowski said. "I don't see a good reason for a respiratory disease to stay in the population longer than necessary."
He then is quoted describing why this approach makes no sense to him:
With all respiratory diseases, the only thing that stops the disease is herd immunity. About 80% of the people need to have had contact with the virus, and the majority of them won't even have recognized that they were infected, or they had very, very mild symptoms, especially if they are children. So, it's very important to keep the schools open and kids mingling to spread the virus to get herd immunity as fast as possible, and then the elderly people, who should be separated, and the nursing homes should be closed during that time, can come back and meet their children and grandchildren after about 4 weeks when the virus has been exterminated.
Wittkowski emphasizes elsewhere the importance of timing. He said this at the end of his study:
Aside from separating susceptible populations (elderly and high-risk subjects, e.g., in nursing homes) from the epidemic, which is effective as long as virus is circulating, public health intervention aiming to contain a respiratory disease need to start within a narrow window of opportunity. ... When the window of opportunity has been missed, any type of containment has only limited impact on the course of the epidemic, but high impact on economy and society.
He warned in the interview, which was conducted at the beginning of April, that herd immunity now is what we need to avoid a second wave of COVID-19. Here's what he said: "[If] we are preventing herd immunity from developing, it is almost guaranteed that we have a second wave as soon as either we stop the social distancing or the climate changes with winter coming or something like that."
Wittkowski also said: "Unfortunately, it seems that in western countries where the story of China was already known, people started with social distancing, as imperfect as it is, before the epidemic could reach the level that is needed to develop herd immunity."
Herd immunity was initally advocated by some, including UK Prime Minister Boris Johnson, who initially refused to ban large gatherings before changing course. (Johnson now has the virus and was in a hospital's intensive care unit at the time of writing.)
The World Health Organization expressed concerns early on about resistance to social-distancing measures. Here are warnings issued by WHO spokeswoman Dr. Margaret Harris, and quoted in this story, in mid-March:
We don't know enough about the science of this virus. It hasn't been in our population for long enough for us to know what it does in immunological terms.
Every virus functions differently in your body and stimulates a different immunological profile.
We can talk theories, but at the moment we are really facing a situation where we have got to look at action.
Until there's a vaccine and more is understood about COVID-19, including whether a person can contract it more than once, Harris and others fear, it's too soon to strive for herd immunity. Plus, at a time when hospital resources are already stretched too thin, it's important to control the spread of the virus.
Healthline laid out "reasons why herd immunity isn't the answer to stopping the spread of the new coronavirus." Here are the thoughts to consider, as listed by Healthline:
- There isn't yet a vaccine for SARS-CoV-2. Vaccinations are the safest way to practice herd immunity in a population.
- The research for antivirals and other medications to treat COVID-19 is ongoing.
- Scientists don't know if you can contract SARS-CoV-2 and develop COVID-19 more than once.
- People who contract SARS-CoV-2 and develop COVID-19 can experience serious side effects. Severe cases can lead to death.
- Doctors don't yet know exactly why some people who contract SARS-CoV-2 develop severe COVID-19, while others do not.
- Vulnerable members of society, such as older adults and people with some chronic health conditions, could get very sick if they're exposed to this virus.
- Otherwise healthy and younger people may become very ill with COVID-19.
- Hospitals and healthcare systems may be overburdened if many people develop COVID-19 at the same time.
This doesn't mean we shouldn't hope for herd immunity down the road.
In fact, Dr. Ariel Pablos-Mendez, a professor at Columbia University Medical Center in New York and former head of global health at the U.S. Agency for International Development, was behind an April 8, 2020, opinon piece in The Hill that promoted that very goal.
In "More herd immunity, less herd mentality," Pablos-Mendez called for the collection of better data in the U.S., which could help free people from lockdown. He pointed to Germany as an example of what is possible:
The Germans are doing massive testing and isolating confirmed cases while ramping up hospital care capacity and incentivizing innovation. Most importantly, they are progressively reopening their economy by issuing "certificates of immunity" to frontline workers and others who test positive for antibodies of the virus (i.e. serology test). A crazy idea? Not if you value both public health and the economy.
The problem is "serology testing has been missing in U.S. data-gathering efforts," he said, adding:
We need to flatten the curve for the elderly but accelerate herd immunity for the healthy so that we don't kill the economy trying to outrun the pandemic in lockdown."
But without the right tests and expanded data, many experts warn we can't safely make that shift.
Updates:
-
2020-04-14T18:18:58Z 2020-04-14T18:18:58Z We have updated the headline to remove the "Fact Check" label, as there continues to be disagreement over the safety and wisdom of lifting lockdowns and stay-at-home orders.