Are health care professionals being "urged" to call vaginas "bonus holes" to avoid offending "trans or non-binary patients"? No, that's not true: There is no widespread or official push to change the terminology. A single charity in the United Kingdom suggested it as an option.
In health care, professionals typically use anatomically correct and medically appropriate terminology when referring to body parts. Health care providers are trained to communicate with patients in a way that is sensitive to their gender identity and expression, using appropriate pronouns and terminology that align with their individual preferences, according to two health care organizations.
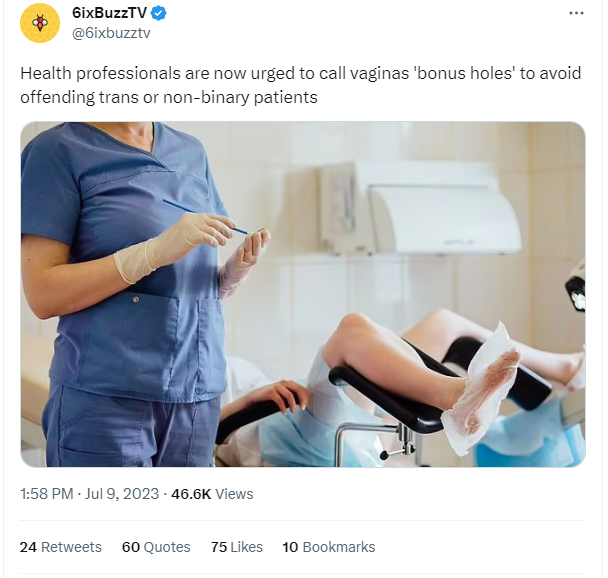
The claim appeared in a post on Twitter (archived here) published by the Canadian media platform 6ixBuzzTV on July 9, 2023. The caption says:
Health professionals are now urged to call vaginas 'bonus holes' to avoid offending trans or non-binary patients
This is what the post looked like on Twitter at the time of writing:
(Source: Twitter screenshot taken on Tue Jul 11 14:50:02 2023 UTC)
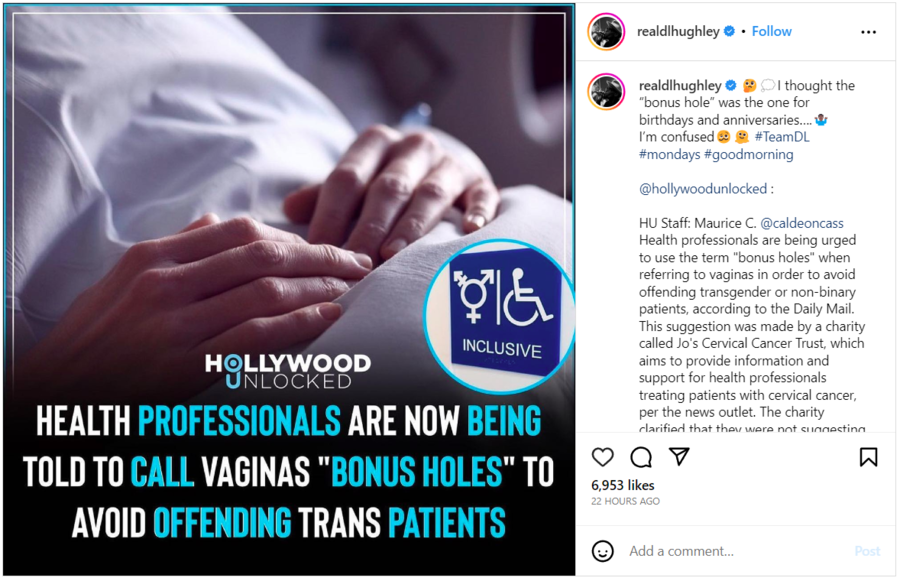
The claim also appeared in a post on Instagram on July 10, 2023. It appears below:
(Source: Instagram screenshot taken on Tue Jul 11 16:27:13 2023 UTC)
American College of Obstetricians and Gynecologists
Rachel Kingery, a senior media relations manager at the American College of Obstetricians and Gynecologists (ACOG), provided this response from the organization about the terminology to Lead Stories in a July 11, 2023 email. It said:
ACOG continues to use the clinically accurate term 'vagina.'
The group's website includes this guidance on Health Care for Transgender and Gender Diverse Individuals, which includes a list of "Terminology and Definitions."
National Coalition for LGBT Health
In a July 11, 2023, email to Lead Stories, Brian Hujdich, executive director of the National Coalition for LGBT Health, offered the organization's response to the post's claim:
Healthcare professionals are not and never have been encouraged to refer to vaginal openings as 'bonus-holes' in order to avoid offending patients who identify as Trans. It is not even an obliquely recognized medical practice or type of best practices terminology to refer to vaginas as 'bonus-holes'. It is important to provide quality healthcare while maintaining patient comfort, communication, and trust.
When communicating with patients, healthcare providers should use inclusive, affirming, and respectful language that is linguistically accurate and appropriate. This includes those who identify themselves as Transgender or even Questioning and Intersex. It is important to use terminology that respects a person's preferences and aligns with their gender identity. It is important that medical terminology be clear, accurate and respectful.
Healthcare professionals strive to create an environment that is welcoming and safe for all patients and it's vitally empowering to use appropriate terminology, as well as address patients using their preferred pronouns and name, in addition to providing culturally sensitive care as a standard of practice.
Jo's Cervical Cancer Trust
The reference to the vagina as a "bonus hole" comes not from a medical entity, but from the U.K. charity Jo's Cervical Cancer Trust. The term appears in a glossary on its website called "Language to use when supporting trans men and/or non-binary people," which the Trust produced with the British-based LGBT Foundation. This is what it says:
Bonus hole - An alternative word for the vagina. It is important to check which words someone would prefer to use.
The glossary also offers this option:
Front hole - An alternative word for the vagina. It is important to check which words someone would prefer to use.
The web page does not urge health professionals to use any of the terms. They are merely suggested options:
This glossary explains some of the words we use in our information or that you might hear used by a patient. This is not a definitive list and we recognise that some people may prefer different words. It is still necessary to check the words or phrases your patient would prefer.
The charity explains its rationale for offering alternative words in a section of its website on "Cervical screening for trans men and/or non-binary people." It says:
Accessing cervical screening in an environment where they feel safe and in control can be difficult for many people. This can be exacerbated for trans men and/or non-binary people with a cervix who may face personal and systematic barriers to accessing routine cervical screening, as well as discrimination because of their gender identity. ...
Anyone with a cervix between ages 25 and 64 is eligible for cervical screening, which includes many trans men and/or non-binary people. Some trans men and/or non-binary people may have had gender confirmation surgery that involves removing the cervix, so will no longer be eligible. Trans women do not need cervical screening.
Read these additional Lead Stories fact checks about claims related to Pride and LGBTQ+ issues.